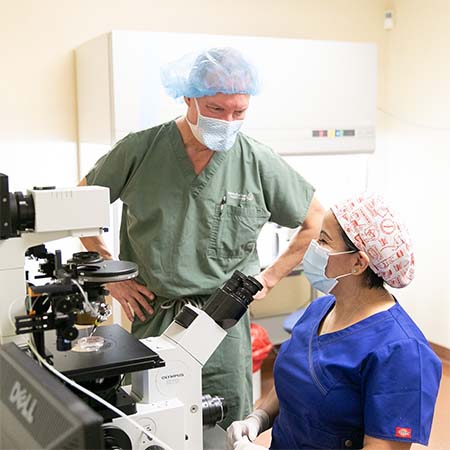
Tubal Ligation Reversal
Many women who have had a tubal ligation–or more commonly known as “having your tubes tied”–find themselves looking to grow their family years after the procedure. While it may seem like having a family or expanding your family is no longer in reach, there are paths you can take that could lead to positive results.
Egg Freezing
Oocyte cryopreservation, or egg freezing, is a method of preserving a woman’s eggs to be used later. It’s usually chosen by women who want children at some point, but don’t want them right now, and who don’t want to risk losing their future ability to have children because they’re waiting.
Embryo Adoption
For couples who successfully have as many babies as they desire through IVF, there’s a choice about what to do with any remaining embryos. They can be discarded, donated to medical research, or offered for adoption. When a couple chooses to offer their embryos for adoption, other couples who have not been successful with IVF using their own embryos can choose to use them in their own IVF cycles.
LGBTQ+ Family Planning
At Reproductive Health Center, we’re dedicated to creating healthy families of all kinds. This is a welcoming environment for all couples, including LGBTQ+ couples, who want to become parents. Technology can offer many options for LGBTQ+ couples to achieve their dream of becoming parents.
Vasectomy Reversal
In many cases, a vasectomy can be reversed using microsurgical techniques. The vas deferens, the tube that carries sperm from the testicle and was cut during the vasectomy, can often be reconnected. This procedure is more complex than a vasectomy; it takes about two to four hours and is usually performed under general anesthesia.
Ovulation Induction
When a woman doesn’t ovulate at all, it’s known as anovulation; when she ovulates irregularly (meaning that she doesn’t ovulate every month), it’s called oligoovulation. These disorders account for about a third of the infertility problems that we see at our Tucson, AZ fertility clinic, and either type can be treated with ovulation induction.